Achilles Tendon Ruptures and Tendinitis
Achilles Tendon Ruptures
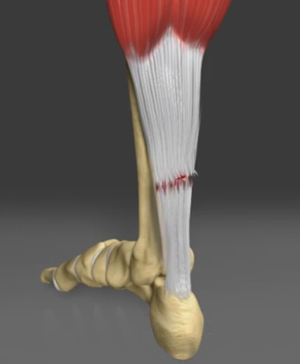
Achilles tendon is a strong fibrous cord present behind the ankle that connects the calf muscles to the heel bone. It is used when you walk, run and jump. The Achilles tendon ruptures most often in athletes participating in sports that involve running, pivoting and jumping. Recreational sports that may cause Achilles rupture include tennis, football, basketball and gymnastics.
When the Achilles tendon ruptures you will experience severe pain in the back of your leg above your heel, swelling, stiffness, and difficulty to stand on tiptoe and push the leg when walking. A popping or snapping sound may be heard when the injury occurs.
Your doctor diagnoses the rupture based on symptoms, history of the injury and physical examination. Your doctor may also feel a gap or depression in the tendon, just above heel bone. Your doctor will gently squeeze the calf muscles. If the Achilles tendon is intact, there will be flexion movement of the foot, if it is ruptured, there will be no movement observed.
Achilles tendon rupture is treated using non-surgical method or surgical method. Non-surgical treatment involves wearing a cast or special brace which lifts your heel, allowing the tendon to heal. Surgical procedure involves opening the skin and suturing the torn tendon together. Surgery helps to decrease the recurrence of the Achilles tendon in comparison to the non-surgical treatment. With either treatment, physical therapy is recommended to improve the strength and flexibility of leg muscles and the Achilles tendon.
To help prevent an Achilles tendon injury, it is a good practice to perform stretching and warm-up exercises before participating in any exercises or sports activities. Gradually increase the intensity and length of time of activity. Muscle conditioning may help to strengthen the muscles in the body.
Tendinitis
Tendinitis refers to the inflammation of a tendon, which is a band of fibrous connective tissue that attaches a muscle to a bone. Tendinitis can result from repetitive or overuse injuries and can occur during activities such as gardening, carpentry, shoveling, painting, scrubbing, tennis, golfing, skiing, and pitching. People with poor posture or those who avoid stretching before exercise are at a higher risk of developing tendonitis. Tendinitis can also affect individuals with rheumatoid arthritis, gout, psoriatic arthritis, thyroid disorders, infections or an unusual medication reaction.
Tendinitis can affect individuals of any age but is more common in adults over the age of 40 years, as tendons lose their strength and elasticity with age, and become susceptible to tear. Tendinitis can affect any tendon; however, it commonly involves the shoulder, elbow, base of the thumb, hip, knee and the heel (Achilles tendinitis).
The predominant symptom is pain at the site of the injured tendon. The pain may occur suddenly or develop gradually and may be severe. The motility of the joint, close to the affected tendon, may also be affected.
The initial treatment of tendinitis includes rest, avoiding activities that worsen the condition, application of ice to the affected area, and anti-inflammatory medications. Corticosteroid injections, physical therapy, and surgery may be considered if the symptoms of tendinitis persist and do not respond to the initial line of treatment. Depending on the severity of the damage, the healing period may vary from a few weeks to months. To decrease your chance of developing tendinitis, avoid repetitive movements; stop any activity that causes pain, and gradually increase your activity levels.
Contact your doctor immediately if you have fever, swelling, redness and warmth to the area, multiple sites of pain, or lack of ability to move the involved area.














